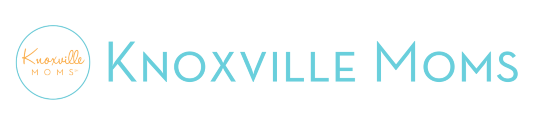 Numerous articles and blog posts have been written about RSV. I see many titled Don’t Touch My Baby or Don’t Kiss My Baby or Don’t Hold My Baby, usually published during the winter when germs come out with a vengeance. I am not here to preach or tell you what to do or not do around newborns. I am purely here to tell you our experience with RSV. Every person’s story with this virus is different except for one fact: it’s scary. Every parent whose child has come down with RSV was scared.
Numerous articles and blog posts have been written about RSV. I see many titled Don’t Touch My Baby or Don’t Kiss My Baby or Don’t Hold My Baby, usually published during the winter when germs come out with a vengeance. I am not here to preach or tell you what to do or not do around newborns. I am purely here to tell you our experience with RSV. Every person’s story with this virus is different except for one fact: it’s scary. Every parent whose child has come down with RSV was scared.
Most babies get to come home. Some babies don’t. That’s how serious this illness is.
Before our scare in 2017, I had never heard of RSV. It is basically a really bad cold, but when newborns catch it, their tiny bodies aren’t strong enough to fight off the virus. What would be a simple cold for anyone else, quickly turns into respiratory distress, bronchiolitis, pneumonia and/or other life-threatening complications for a baby. First signs could be a forceful cough, bad congestion, drop in temperature, lethargy, or sometimes, stopped breathing.
My pregnancy with our third child was normal except that he arrived 26 days premature, exactly two weeks before Christmas. Although he was early, he was already a healthy size at 6 lbs 5 oz. Over the next two weeks, he would randomly cough a single forceful cough, which I thought sounded weird, but I just figured that was his personalized cough sound. He had also been congested, but I knew he probably had a cold because I had had a bad cold during my recovery and he basically lived under my nose for feedings. He also slept more than my prior babies, but I figured that was due to his early arrival. So many signs were there, but I found a reasonable explanation for each, plus I mentioned all of this at his doctor visits, but no one seemed concerned as he always checked out healthy.
The morning after Christmas, he had his two-week check-up with the pediatrician. Once again, he checked out fine; she only mentioned that his temperature was a little low so to keep him wrapped up and warm. His next two feedings were very unsuccessful due to increased lethargy, but the pediatrician told us to start supplementing with formula that day, so I figured he was just getting full faster and not hungry.
My husband, seemingly more worried than me, bundled him up even more and held him while I tended to housework and our other two kids. Overhearing some panic later, I came downstairs to check on things and my husband said our son had turned blue, his eyes had rolled back and he possibly stopped breathing, but was now breathing again and looking normal. He handed him to me and he immediately let out a loud cry and seemed fine. Having just had a well visit at the doc that same day and my son seeming fine to me, I questioned my husband’s worry, but hearing the panic in his voice and seeing it in his eyes I said, “If you feel like something is wrong let’s take him somewhere.”
On the way to the ER, I reached back to touch whatever part of him I could from the front passenger seat. Only now, in retrospect, does the sound coming from him haunt me. At the time, I felt like any sound at all at least meant he was breathing. But later, when thinking about the sound he was making, I realized it was only air being expelled. At the ER, they took him back immediately, but at that point I had not personally witnessed any concerning behavior from our son. It wasn’t until I was holding him while waiting for the ER doctor that his head went limp, his face immediately turned blue and his eyes rolled back in opposite directions that I saw what my husband had seen. I ran out to the hallway holding him yelling for help, when a passing nurse came in, looked at him and left running. A doctor ran in and began pumping his little legs up into his chest.
The room had a wall jutting out in the middle, creating two alcoves. I stood alone in one alcove, crying, shaking, eyes darting around at what was happening, as my husband and two daughters stood in the other alcove probably doing the same thing.
I can still feel the aloneness those two alcoves created.
Once they got my son breathing again, they carried him across the hallway to the trauma room where there were so many people around his table we couldn’t even see him anymore. They gave him a shot of epinephrine which is basically like pumping adrenaline into the body to improve breathing, get the heart rate back up and help stabilize blood pressure.
At some point during all of this, we found out his temperature was 92F degrees. For reference, moderate hypothermia falls in the range of 95-93F degrees. Core temps of 92F and below are life-threatening. As a nurse explained to us, his body was basically putting his organs on ice to protect them because his body was shutting down. He was wrapped in warming blankets and wheeled up to the NICU where we were told the best thing we could do was go home and get some sleep. This was the last thing we wanted to do, but they promised to call with any changes. He only had one more apneic episode that night, but needed a week of recovery as we also discovered he had bronchiolitis and possible pneumonia.
Transmitting RSV to other sick NICU babies can be deadly to them, so he was placed in the tiny isolation room with space for only one baby isolette and a chair for me. Ironically, although he was fighting for his life, he was the threat.

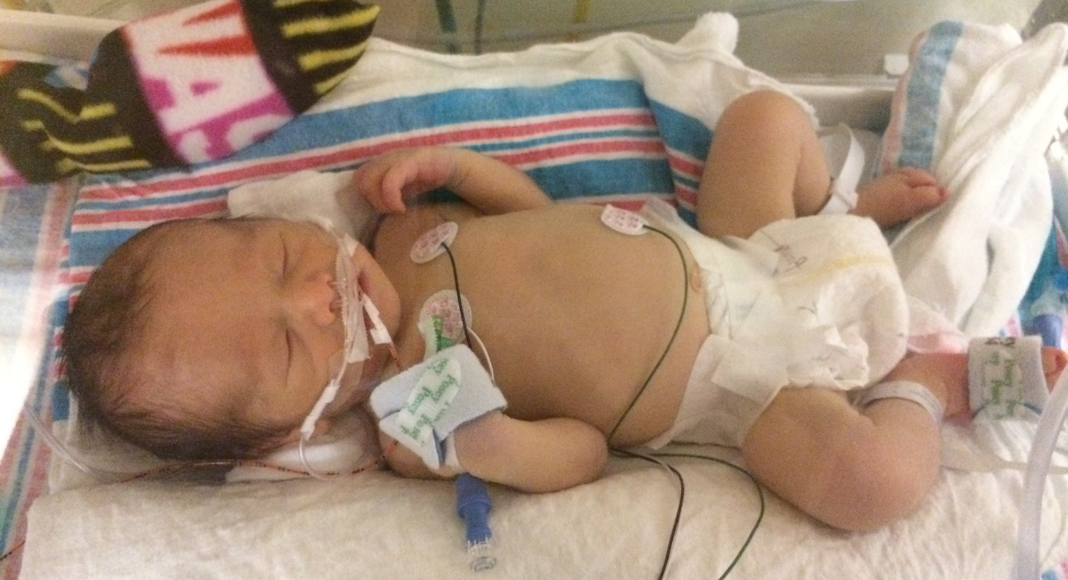
Looking at him hooked up to the breathing tubes and feeding tubes and other tubes, I didn’t recognize the baby I had just brought home from the hospital two weeks ago. With around the clock care he fortunately improved and each day another tube was removed from his tiny body, a little more color came to his cheeks, I saw his eyeballs a bit more, and he slowly returned to the baby I had brought home.
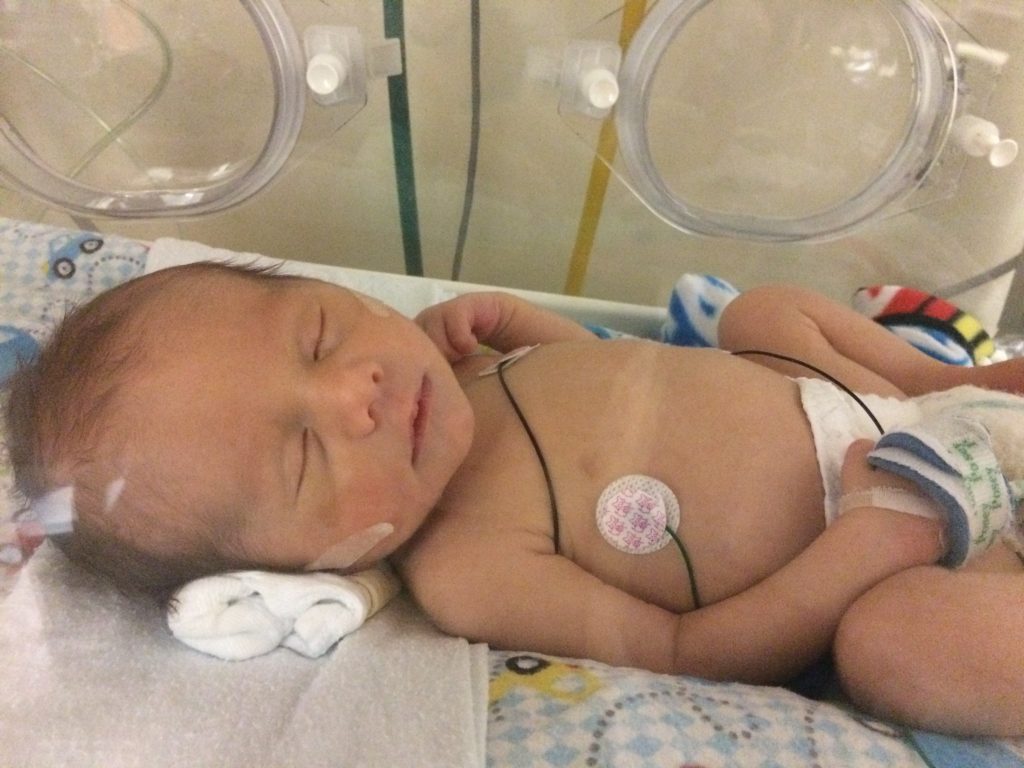
On day five, we moved across the hall to our own hospital room to ensure he could remain stable on his own for two days. We celebrated New Year’s Eve by watching the ball drop, just the two of us. We were so grateful he entered 2018 with us.

If you ever have concern over your baby’s cold and you see these signs, consult with your pediatrician to prevent further complications. RSV can hit hard and fast. Remember, our son checked out fine with the pediatrician six hours before we raced to the ER. At the hospital, we were told he would not have made it through the night.